Translate this page into:
Spinal cord compression secondary to vertebral echinococcosis
Address for correspondence: Prof. Knut Wester, Department of Clinical Medicine (K1), University of Bergen, 5021 Bergen, Norway. E-mail: kgwe@helse-bergen.no
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
We describe a patient with progressive lower limb weakness and paresthesia 3 days after falling from a considerable height. Magnetic resonance imaging and computed tomography revealed collapsed Th2 and Th3 vertebrae. A tuberculous (TB) spondylitis was suspected, and anti-TB medication was started however with no clinical improvement. She was referred to our center and operated. A 3 level discectomy and 2 level corpectomy were performed with iliac bone grafting and anterior plating via an anterior cervical approach. The patient developed an esophagocutaneous fistula that was repaired and cured. The biopsy specimen showed a hydatid cyst of the vertebra as the cause of the lesion. After the result, she was started on oral albendazole. At follow-up nearly 4 months after surgery, the patient had regained significant power in her lower limbs with a muscular strength of 5/5 in both legs, thus making it possible to walk without support.
Keywords
Cystic echinococcosis
hydatid disease
tuberculous spondylitis
Introduction
Hydatid disease or cystic echinococcosis (CE) is caused by the larval stage of the cestode Echinococcus granulosus or Echinococcus multilocularis. It is a disease endemic to many sheep-raising countries.[1] It commonly affects the liver and lungs (60% and 20%, respectively) but may also rarely have an intracranial location: About 1–2% of all cases. Bone hydatid disease is similarly uncommon, seen in 0.5–4% of CE cases. Of the bones, the spine tends to be involved in 50% of cases and of these; the thoracic spine in about half.[2] The femur, pelvis, humerus, ribs, and tibia may also be affected, in descending order.[1] CE usually presents as a slowly growing mass, with a rate of 1 cm/year. Spinal CE, which can be classified as intramedullary, intradural-extramedullar, extradural-intraspinal, vertebral, and paravertebral (including dumbbell) processes, is associated with high mortality and morbidity. Comprehensive reviews of spinal hydatidosis have been given by Bhake and Agrawal and Neumayr et al.[34]
Case Report
The patient is a 20-year-old female patient who was admitted to our hospital 6 weeks after a fall from the 3rd floor of a building; she landed on her feet and subsequently fell on her back. She experienced immediate upper back pain but was ambulating for the next 3 days, and then she developed weakness of the lower limbs, initially most prominent on the right side. A tuberculous (TB) spondylitis was suspected after computed tomography (CT) and magnetic resonance imaging [Figure 1] showed collapsed Th2 and Th3 vertebrae and compression of the spinal cord with associated paravertebral processes. Consequently, she received anti-TB medication and prednisolone for the next 4 weeks in another hospital, however with no clinical improvement. To the contrary, she also developed decreased sensation below the chest and numbness that later developed into dysesthesia. She was still continent to urine and feces. The weakness progressively worsened and developed into a bilateral total paraparesis.
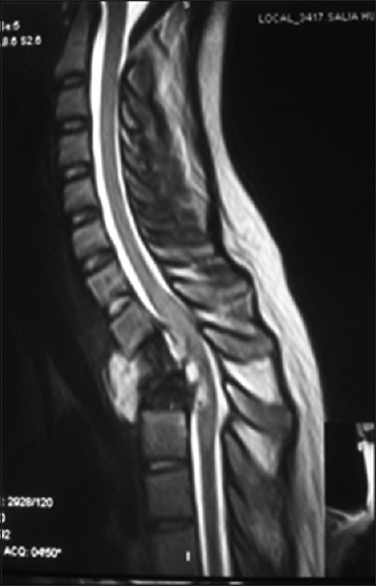
- T2-weighted image showing destruction of Th2 and Th3 vertebra and the associated intervertebral discs
On admission to our hospital, she had complete loss of power and muscular tone in the legs, with the exception of some rotation in the right hip joint, with exaggerated reflexes. In addition, she had decreased sensation to pain and temperature in both legs.
Surgery
Still under the presumption that she had a TB spondylitis, she was operated via a left cervical incision (the left side is preferred to reduce the chance of recurrent laryngeal nerve injury). The mass was approached, and three level thoracic discectomy (Th1-Th2, Th2-Th3 and Th3-Th4) and two level corpectomy (T2 and T3) were performed. Large iliac bone grafts were taken and grafted along with anterior fixation. Postoperatively, the patient was stable, but there was no immediate change in her clinical condition with regard to power and sensation. She developed a wound leak with discharge of ingested matter, indicating an esophageal fistula. A tear in the posterior esophagus could be identified, and she was reoperated. A nasogastric tube was inserted under direct vision, and the wound was repaired without complications. The biopsy specimen revealed hydatidosis of the spine.
Follow-up
Postoperatively, the patient stayed in hospital for 3 weeks with nutritional and rehabilitation care. At follow-up nearly 4 months after surgery, she had regained muscular strength completely in her lower limbs, thus she walked without support. Postoperative X-ray and CT imaging at 3 months [Figures 2 and 3] showed an acceptable graft alignment with screws and plate in place.
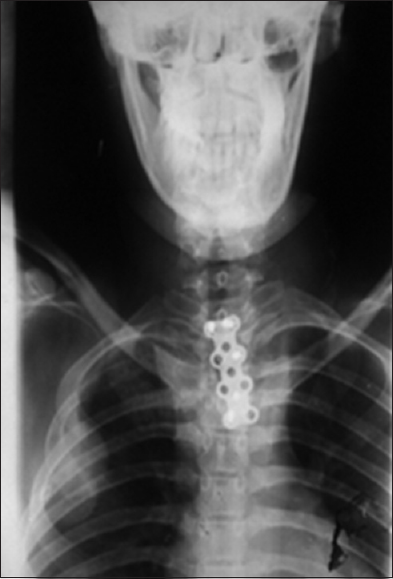
- Postoperative X-ray showing position of plate
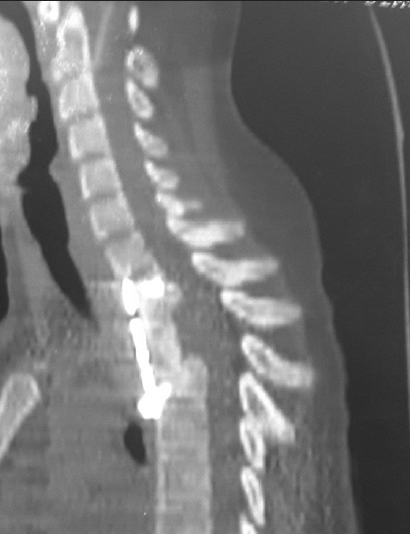
- Postoperative, sagittal reformatted computed tomography scan showing restored axial alignment and position of plate
Discussion
Here, we have presented a patient with CE, inflicting on and destroying thoracic corpora. CE patients with the affection of bone usually present with pain (41.5%), paraplegia (22%), and pathological fractures (48%). Pathological fractures are most frequently found in the spine (75.0%) followed by the femur (20.0%) and tibia (5.0%). However, 19.5% of patients do not develop any complications or symptoms.[1] Our patient presented with the 3 most common symptoms: A pathological fracture, pain, and progressive paraplegia.
Intraosseous foci of hydatid disease predominate in spongious bone tissue and consist of small, separate, and thin-walled cysts. When these cysts expand, they destroy the surrounding trabeculae and can reach a considerable size. Due to cyst enlargement and consequent cortical thinning, pathological fractures may occur.
Diagnosis
Radiological diagnosis of osseous hydatid disease is difficult because of the rather nonspecific findings, explaining how our patient could be misdiagnosed as having TB. Radiography usually reveals single or multiple osteolytic lesions and in some cases shows cortical thinning, osteosclerosis, and pathological fractures, thus making it difficult to distinguish the condition from TB spondylitis or chronic osteomyelitis.[15] In the case of connective tissue proliferation and bone sclerosis, bone CE can radiologically present itself as a tumefaction. Extraosseous cysts may calcify, whereas intraosseous disease rarely demonstrates calcification.[15] In some cases, presentation of CE can be unclear, consisting of mixed radiological signs.
Treatment
The treatment of spinal CE can be surgical and/or medical. Here, we will emphasize the surgical treatment. The rapid development of neurological symptoms leading to early diagnostic work-up and surgery is considered to be important for a favorable outcome, especially when the lesion is a single cyst.[14] Complete and unruptured excision is the goal, but this may be difficult in vertebral lesions. If possible, radical surgery is advocated, and although often not precluding disease progression, it has been shown to prolong survival in selected cases. The location and the extent of the lesion(s) determine the surgical approach and procedure.
Intradural and extradural extraosseous lesions are approached by posterior laminectomy followed by durotomy[14] with the aim to cure. Complete resection of these cysts without rupture is the goal of the procedure and will be feasible and curative in most cases, even in the presence of adhesions to surrounding tissue.
Vertebral lesions are more complicated. For lesions affecting the stability of the spine, a wide spectrum of techniques has been employed after resection of affected bone to stabilize the vertebral column (including bone grafts, dorsal stabilization by pedicle screw systems, plating, and a variety of other fixation techniques). However, there are not enough data to recommend the use of any specific technique.[4]
Medical treatment consists of the use of benzimidazoles. Data on the efficacy of benzimidazoles in osseous CE are scarce, and the contribution of these drugs to cure or even prevent recurrence in vertebral CE is frequently debated. It is well-accepted that larger cyst size and the presence of daughter cysts, especially bone involvement is unfavorable. In a study of 40 patients with inoperable vertebral hydatidosis, a cure rate of 53% with albendazole treatment at a minimal follow-up time of 2 years was reported. The successful medical treatment of a residual cyst (postsurgery) with a 1-year course of albendazole has been reported (follow-up time at publication: 1 year).[4]
Prognosis
The prognosis is dependent on at least 3 separate conditions, the recurrence rate (RR), the extent, speed, and duration of the neurological impairment, and finally: The effect of the treatment. The RR ranges from 0% to 100% depending on the site of the lesion.[14] Intraspinal lesions have the lowest RR of all manifestations. The two main factors determining recurrence (complete and unruptured resection) might explain the higher RR of extradural-extraosseous CE. This holds true for vertebral lesions as well. The infiltrative nature of the microvesicular lesions does not allow for unruptured resection of the cysts and leakage of their contents is, therefore, inevitable.[4]
Patients with cysts that affect the intradural space typically present with symptoms due to acute or subacute compression of the spinal cord requiring urgent surgical decompression to avoid permanent and severe neurological impairment. Our patient had already lost all muscular power and tonus in the lower extremities and was lucky to regain her neurological functions after so long time. The relatively favorable outcome was most probably due to the fact that the spinal cord damage was incomplete; she still had sensory functions and was continent at the time of surgery.
Conclusion
Spinal CE is a rare disease that is a one of the rare causes of compressive spinal pathology. It should be considered as a differential in endemic countries. It is treated both medically and surgically, surgery being the treatment of choice. The mortality is still high with high RR even after treatment.
Source of Support: Nil.
Conflict of Interest: None declared.
References
- Skeletal manifestations of hydatid disease in Serbia: Demographic distribution, site involvement, radiological findings, and complications. Korean J Parasitol. 2013;51:453-9.
- [Google Scholar]
- Spinal cystic echinococcosis – A systematic analysis and review of the literature: Part 2. Treatment, follow-up and outcome. PLoS Negl Trop Dis. 2013;7:e2458.
- [Google Scholar]
- Hydatid disease: Radiologic and pathologic features and complications. Radiographics. 2000;20:795-817.
- [Google Scholar]






