Translate this page into:
Purple glove syndrome: A looming threat
Address for correspondence: Dr. S SenthilKumaran, Department of Accident, Emergency & Critical Care Medicine, Sri Gokulam Hospital & Research Institute, Salem, Tamil Nadu, India. E-mail: maniansenthil@yahoo.co.in
This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3.0 Unported, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This article was originally published by Medknow Publications and was migrated to Scientific Scholar after the change of Publisher.
Sir,
Phenytoin is a nonsedative, broad-spectrum anticonvulsant drug that has been used in the treatment and prevention of seizures for decades. Intravenous (IV) administration of phenytoin with or without extravasation can result in a devastating complication called as “Purple Glove Syndrome (PGS)” for its characteristic purplish-black discoloration accompanied by edema and pain distal to the site of injection.[1] Here we report a case of PGS following extravasation of phenytoin so as to alert clinicians on this potentially serious injury and suggest the ways to prevent it. A 60-year-old woman was admitted in a peripheral hospital for frontal bone fracture following road traffic accident (RTA) with normal brain parenchyma and generalized tonic-clonic seizure, for which she received 900 mg of loading dose of phenytoin dissolved in 100 ml of normal saline through a 22-gauge peripheral intravenous catheter kept in her left dorsum of the hand over 45 minutes. Two hours later, the patient's left hand was swollen and became bluish in color. The patient complained of severe pain at the site of injection, which soon spread throughout the left hand. On examination, the patient's left hand and forearm were edematous and had purplish-blue discoloration without blisters, cool to the touch [Figure 1] and tender. The radial pulse was feeble and the capillary refill was sluggish and pulse oximeter applied showed a good trace. Duplex ultrasound of the upper limb showed normal flow. A working diagnosis of PGS, possibly due to the extravasation of intravenous phenytoin, was made. Compartment syndrome was ruled out.
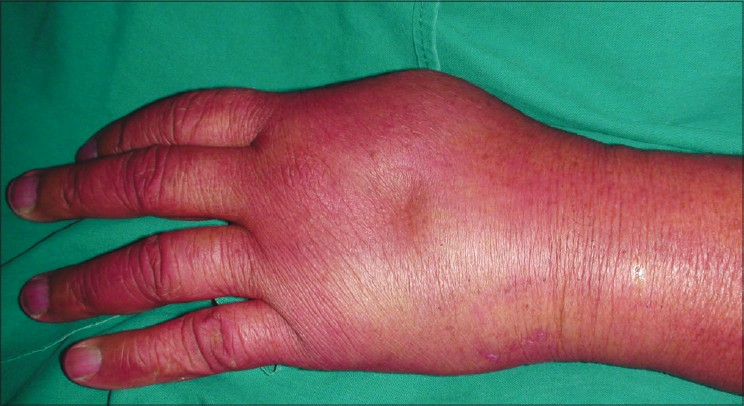
- Left hand was edematous and had purplish-blue discoloration without blisters
The IV access was removed. The arm was kept elevated and dry heat was applied. Topical nitroglycerin patch was kept. Since the pain was intense and was not relieved with parental nonsteroidal anti-inflammatory drugs, brachial plexus was blocked. The swelling subsided after 72 hours and the discoloration started disappearing from the periphery. The patient got discharged after 5 days. Her anatomical and functional aspects of hand and fingers recovered well without any squeal, over a period of 2 weeks. Extravasation of injected drugs may result from a simple phlebitis to soft tissue necrosis. Certain factors like age, level of consciousness, venous circulation, location of the IV cannula and chemical characteristics of the drug (high osmolality or vesicant properties) determine the severity of the injury. The prevalence of PGS following intravenous administration of phenytoin varied from 1.7 to 7%.[23]
The pathophysiology of PGS is poorly understood. However, it may be related to the crystallization of phenytoin upon contact with blood and extravasates into the interstitial tissue.[4] Another mechanism is due to the disruption of the endothelial–intercellular junctions following leakage of phenytoin and irritation of soft tissue. To obscure the assumption on the etiology even more, the report on PGS occurring after an oral dose[5] of phenytoin suggests that this event may be due to phenytoin itself and not directly related to the infusion. The diagnosis of PGS is mainly clinical based and has three stages. The management is mainly conservative, if circulation is preserved. Due to widespread use of phenytoin, students of health sciences, practitioners and nurses shall be taught on this entity, and trained to administer phenytoin carefully in order to prevent this episode/event.
References
- Purple glove syndrome: A complication of intravenous phenytoin. J Neurosci Nurs. 1992;24:340-5.
- [Google Scholar]
- Incidence and clinical consequence of the purple glove syndrome in patients receiving intravenous phenytoin. Neurology. 1998;51:1034-9.
- [Google Scholar]
- A prospective study of the incidence of the purple glove syndrome. Epilepsia. 2001;42:1156-9.
- [Google Scholar]
- Extravasation injury of the upper extremity by intravenous phenytoin. Anesth Analg. 2002;94:672-3.
- [Google Scholar]
- Purple glove syndrome caused by oral administration of phenytoin. J Child Neurol. 2000;15:762.
- [Google Scholar]





